In the mountain highlands of western Uganda, Kikanda Batelemao, a community health worker, walks along a rugged dirt road to visit Florence Mbambu, a pregnant woman living more than 35 miles from the nearest health clinic. With every step he takes, he is helping to lead a healthcare revolution: a revolution that is transforming healthcare delivery in some of the poorest and most remote places on earth.
In his pocket, Kikanda carries an old cellphone, but on that simple phone he carries the means to bring new hope to the patients he visits. That phone carries with it the possibility to make healthcare accessible to everyone, no matter where they live or how little money they make.
A Vision of Mobility
Located just north of the equator, nestled deep in the Rwenzori Mountains of western Uganda, is Bwera General Hospital. Bwera is a public hospital administered by the Uganda Ministry of Health. Here, in one of the poorest but most spectacularly beautiful places on earth, extremes abound. The ratio of doctors to patients is just 1:100,000. Paved roads are few and far between. Electricity is a luxury enjoyed by only a few. But almost everyone, in even the tiniest and most remote villages, owns a cellphone. And cellphone towers are ubiquitous, marching across the landscape in every direction.
For Josh Nesbit, a premed student working one summer at a clinic in Malawi, Africa, the sight of those cell towers would change his life. As he watched pregnant women walk 50 miles or more to see the single doctor in his rural clinic, he also noticed that his cellphone got better reception than it did in San Francisco. Nesbit realized he could use that insight to fundamentally transform and improve healthcare delivery in Africa and other developing nations. The result of that epiphany is Medic Mobile, the organization Nesbit co-founded after returning to the United States in 2009.
There are a billion people who lack access to healthcare. There are 300,000 women who will die in childbirth this year. And there are at least 10 countries where one in four children will not live to age five. Those are all linked, and they are all unacceptable. Being poor should not mean that you have poor healthcare.
JOSH NESBIT, CEO, MEDIC MOBILE
Transforming Healthcare Delivery
Kikanda Batelemao is a community health worker, referred to locally as a VHT, for Village Health Team. VHTs are the cornerstone of Uganda’s primary healthcare model for the millions of Ugandans who live outside the country’s major cities and towns. Just a few years ago, Batelemao would have to travel 35 miles each way, from the tiny hospital in Bwera to the remote mountain communities he serves, to visit his patients and report on their health.

For pregnant women, who are often forced to walk 30 to 50 miles through the densely forested mountains to see a doctor, the situation is particularly dire. A lack of basic education, access to prenatal care, and communications lead to what Dr. Danny Devito Gotto of ACODEV, a non-governmental organization that works in Bwera for the VHT program, calls “the three delays.” These are the three main reasons that Uganda has one of the world’s highest rates of infant mortality and women dying during childbirth. “Women are too busy because they are working in the fields,” Gotto says. “They don’t have the time to walk the many miles to the clinic for prenatal care. And they don’t make a decision until there’s a danger sign, and then, it’s often far too late.”
But today, that situation is changing rapidly because of the tools developed by Medic Mobile to help front-line health workers like Batelemao. Batelemao carries with him a simple cellphone. It operates on a 2G cellular network, the same as many of his patients, including Florence Mbambu, who is pregnant with her third child. On Batelemao’s cellphone is an easy-to-use app developed by Medic Mobile that allows him to register and track the progress of Ms. Mbambu’s pregnancy, communicate reminders to her about her prenatal care and visits to the Bwera Hospital, and monitor her birth outcome.
Instead of having to walk the 35 miles to Bwera Hospital to deliver the information he’s collected about the state of Florence Mbambu’s pregnancy, Batelemao now uses the Medic Mobile app to send a text message, in real time, to the hospital staff.
The hospital analyzes the data sent by Batelemao and automatically sends him back a text message containing any medical updates he needs—which includes, on this particular day, the happy news that Florence Mbambu is due to deliver her baby on March 9, 2016. Batelemao uses this information to explain to her that she should leave her village for the Bwera Hospital in enough time to safely give birth. Later, the automated medical system will send Batelemao an alert to remind him again when Ms. Mbambu’s baby is due.
Before Medic Mobile entered the picture, only 28% of Ugandan women had prenatal care. In just a few years, that figure has risen to 48% and continues to rise. Women are consistently delivering healthy babies and are far less likely to lose a child or suffer potentially life-threatening complications. For Florence Mbambu, the lesson is clear: “I pray that Medic Mobile should come to everywhere in Uganda,” she says, “because it assists us women in giving birth to healthy children.”
And for Kikanda Batelemao, it means that he can spend more time visiting patients, collecting and instantly relaying the life-saving information he collects from his patients in their distant communities.

Medic Mobile field trainers educate community healthcare workers on how to install dual SIM cards and run Medic Mobile software on their phones.

Kikanda Batelemao shares stories with a pregnant mother in a village outside Bwera, Uganda. The bond the healthcare workers form with the mothers in the rural villages of Uganda creates lifetime friendships.

Kikwaya Samson hikes miles across a rural countryside under the cover of robust cellular radio service to visit his patients.
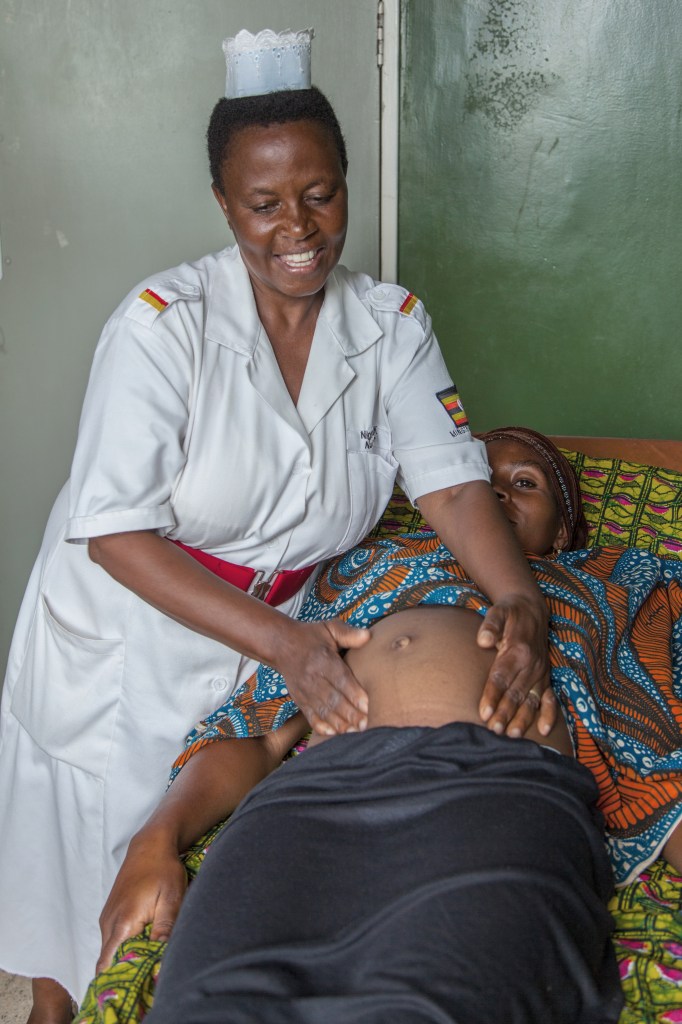
Kyalimpa Specioza is a midwife at Bwera Hospital. She uses the information gathered by the Village Healthcare Technician (VHT) to handle checkups when mothers visit the hospital.
The genius of the Medic Mobile approach lies in its simplicity. “For those of us who work in these communities,” says Dr. Danny Devito Gotto of ACODEV, “we need something that is simple to use, cheap to use, and readily available. We have mobile phones,” Gotto continues. “We have community health workers. We have clinics. The problem is linking the three together. That is what we love about Medic Mobile.”
Nesbit, Medic Mobile’s CEO, realized that a cellphone could dramatically transform healthcare because it allowed community health workers in remote villages to communicate, in real time, with the rural clinics they served. But there was a technical challenge that needed to be overcome first. The problem was how to deliver the healthcare platform to everyone who needed it. “We realized that we couldn’t possibly support every deployment,” Nesbit says. “We needed to make the software radically accessible to any clinic anywhere that needed the tools to be successful.”
The solution Medic Mobile devised was to build a mobile healthcare management system that could be installed in a snap on a mobile phone, and runs on a Linux-based VMware desktop virtualization platform. It hosts the Medic Mobile software tool kit, a tool kit that combines smart messaging, decision support, easy data gathering and management, and health system analytics. The result is a variation on the concept of software as a service (SaaS). As Nesbit says, it is instead "Software Is a Service.”
Working with VMware, Medic Mobile developed a modified SIM card (often made with a tool as simple as a pair of scissors) that can be inserted into any regular cellphone manufactured after 1992. Medic Mobile calls the device a parallel SIM card. This hardware device is a microcontroller that allows the community health worker to run the Medic Mobile software tool kit apps.
VMware enables the Medic Mobile tool kit to be used in almost any kind of environment, support any language, and work with or without internet connectivity, locally or in the cloud. Medic Mobile also uses the VMware virtual infrastructure extension (VIX) to automate the delivery of its healthcare apps where internet connectivity makes that possible. VIX allows the Medic Mobile system to automatically send and receive SMS (text) messages over any cellular WiFi network.
Working with VMware engineers, Medic Mobile designed these tools to work on the simplest of mobile platforms: the inexpensive cellphones that are widely available even in the poorest countries of the developing world.
It’s not medical innovation. It’s a system innovation and a delivery innovation. It’s rethinking who’s providing care for whom.
JOSH NESBIT, CEO, MEDIC MOBILE
Envisioning Global Health Equity
More than 10,000 health workers in 23 countries in Africa and Asia use Medic Mobile’s tools today. These 10,000 health workers care for more than 5 million people living in the poorest and remotest places on earth. But Nesbit is not satisfied. “We have really ambitious five year goals,” he says. “By the year 2020, we want to be supporting 200,000 health workers and improving healthcare for at least 100 million people.”
Medic Mobile is driving a revolution in healthcare delivery by addressing the most critical delay for millions of people worldwide: their decision to access healthcare. As Dr. Danny Devito Gotto of ACODEV explained earlier, the ability to communicate healthcare data in real time makes a tremendous difference, often between life and death. Because of this, Gotto says, “Medic Mobile is the future of healthcare in Africa.” The same could be easily said about Asia and the poorest and most remote communities of North and South America, as well.
Nesbit says that Medic Mobile is taking advantage of what he calls a “really amazing moment in human history, where a new technology and a new infrastructure was spreading faster than anything we had ever seen before.” The conjunction of mobile technology and the cellular tower infrastructure was that moment. On that summer day in Malawi, Nesbit realized its potential and resolved to act. Medic Mobile’s mission is to ensure that potential comes to full fruition.
“Our vision,” Nesbit says, “is that the things that we know save lives should be made accessible to everybody, no matter where they are, no matter how much money they make, no matter to what social group they belong. The vision is global health equity.”
Nesbit asks of us, “Who is a health worker?” He than answers that anyone working to break the stubborn link between poverty and poor health is a health worker. Medic Mobile’s slogan is one that proclaims what the solution is: “We are all health workers.”

